كتاب روابط اجتياز لـ منصة منظمة الصحة العالمية لتبادُل المعارف بشأن السل

3.1.1 Whom to screen for TB
WHO recommends systematic screening for TB of people with a risk factor, who are either seeking health care or who are already in care in settings where TB prevalence among the general population is 100/100 000 or higher and diabetes is listed as one of the risk factors (26). In settings with a TB prevalence of < 100/100 000, TB screening of people living with diabetes may be conducted according to local needs and policies and is an opportunity to advance the TB elimination agenda.
3.1.2 When to screen for TB
There is limited evidence on the optimal timing and frequency of TB screening among people living with diabetes, but studies suggest that people with glycaemic control are at lower risk of TB disease (97–99). Screening of people for TB when they are first diagnosed with diabetes and when they have uncontrolled glycaemia should therefore be a priority. Where the yield of TB screening among people living with diabetes is low, other targeted approaches may be considered. These may include screening for risk factors such as poor glycaemic control, male sex, older age, and lower body mass index (BMI), which could be used to inform a decision on whether to screen for TB (100).
3.1.3 How to screen for TB
Clinically, people living with diabetes are more likely to be sputum smear-positive, to have more extensive and bilateral pulmonary disease, more cavities, larger lymph nodes and atypical findings of lower lobe lesions, especially if they have poor glycaemic control (101). This will affect how best to screen for and diagnose TB in this population.
The baseline assessment of people with newly diagnosed diabetes should include the following questions:
- Is the individual on TB treatment?
- Have they been diagnosed with TB or are they undergoing investigations for TB?
- Have they had TB in the past?
- Has anyone in the household been diagnosed with TB?
If the individual is not already undergoing investigations for TB or on TB treatment, they should be screened for TB when national policy indicates. Those who have symptoms of TB, are undergoing investigations for TB or are on TB treatment should be attended to according to local infection control protocols (see section 3.7). Individuals who are symptomatic should undergo additional investigations to ensure early diagnosis or to rule out TB disease.
WHO-recommended TB screening tools include symptom screening for clinical features associated with pulmonary TB (including prolonged cough [sometimes with blood], chest pain, weakness, fatigue weight loss, fever or night sweats) and screening with chest X-ray (CXR) or a molecular WHO-recommended rapid diagnostic test (mWRD). CAD software programmes may be used in place of human readers to interpret digital CXR for screening and triage for TB disease among individuals aged ≥ 15 years (26).
Table 2 shows the accuracy of these tools in studies of general populations with negative or unknown HIV status and with unknown diabetes status, from a systematic review conducted in 2020 for the update to the WHO TB screening guidelines, with bacteriologically confirmed pulmonary TB as the reference standard (102). It should be noted that most data on the accuracy of screening tools derives from TB prevalence surveys in which the general population in high-TB burden settings are screened for TB.
Table 2. Diagnostic accuracy of symptoms, CXR and mWRDs for screening for TB disease among individuals aged ≥ 15 years with negative or unknown HIV status
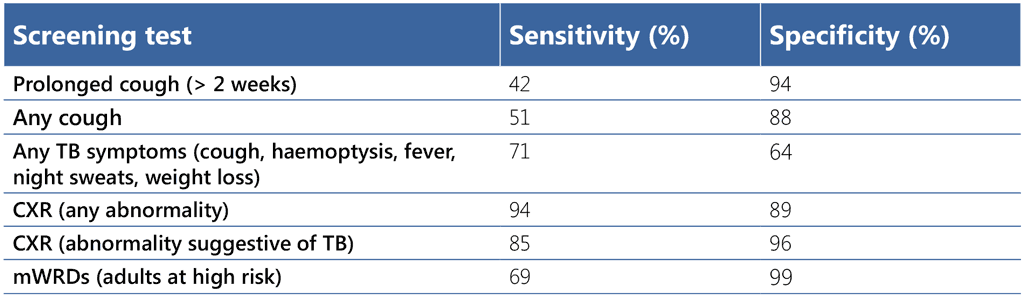
Several studies have been conducted on the yield and accuracy of different TB screening strategies among people living with diabetes, but there is considerable heterogeneity in the findings. This is probably due to differences in the populations tested, the TB prevalence, the screening tools and the procedures used for diagnostic confirmation. Only a few studies provided information on the sensitivity and specificity of different TB screening strategies among people living with diabetes. In line with findings from TB screening studies in the general population, evidence from noncomparative studies shows the limited sensitivity of symptom screening alone as compared with symptom screening combined with CXR in people living with diabetes (103–106). Similarly, evidence suggests that use of a parallel screening algorithm that includes symptom screening and CXR may be a higher-yield strategy than symptom screening alone (107). Results from studies of the use of CAD in people living with diabetes have been promising, and this technology offers an opportunity to expand access to CXR (105,106). Given that people living with diabetes have a high risk of TB, access to technologies such as CXR and CAD is an important consideration for strengthening TB screening in this population.
Selection of the tools and algorithms for TB screening should take into account the extra human and financial resources required to prepare for, carry out and monitor screening activities and to accommodate the increased demand for diagnostic confirmation of people with presumptive TB and the extra number of people who may be identified with TB as a result of screening. The ScreenTB platform (https://screentb.org/) is an interactive tool created by WHO to help users to assess and implement TB screening strategies in various at-risk populations, including people living with diabetes.
3.1.4 Increasing access to TB screening for people with diabetes
Barriers to TB screening among people attending diabetes care include lack of access to sensitive screening modalities such as CXR, poor awareness about the diabetes-related risk of TB by healthcare workers and by people living with diabetes, lack of training and expertise in identifying TB symptoms, stigmatization associated with TB, and poor recording, reporting and referral systems, with inadequate follow-up (108). Key considerations for improving access to TB screening are listed in Box 4. National programmes for TB and NCDs should map and identify appropriate entry points for TB screening among people living with diabetes and develop joint strategies to increase access and build capacity for TB screening of people in diabetes care. The private health-care sector also plays a critical role in providing services for people living with diabetes and may provide an entry-point to TB care and treatment for people seeking care in the private sector.
To determine which cadres of staff should be involved in screening, current terms of reference, workload and the capacity of different staff should be reviewed, including for front-line screening, for managing commodities and supplies (e.g. equipment, software, consumables) and for supervision. Experience in screening people living with diabetes for TB in health facilities can be shared to support implementation of TB screening in other settings. There may be opportunities for remunerated task-sharing and task-shifting by involving people living with diabetes, who could be trained in mobilization or in some screening activities. The model of staffing and supervision will depend on the context, such as urban or rural settings and targeted risk groups.


 تعليق
تعليق