Liens transversaux de livre pour PLATEFORME DE PARTAGE DES CONNAISSANCES SUR LA TUBERCULOSE DE L'OMS
4.2.1 Management of type 2 diabetes
For people with diabetes and TB, the priority is to treat both diseases successfully. Initial management of newly diagnosed type 2 diabetes depends on the symptoms and blood glucose levels. Individuals with symptoms and a fasting plasma glucose ≥ 15 mmol/L or fasting or random plasma glucose > 18 mmol/L, regardless of symptoms, should be tested for urine ketones, diabetes medication should be started, and they should be referred to higher-level care as necessary. For people who have moderately elevated blood glucose levels (fasting plasma glucose [FPG] ≥7 mmol/L and <18 mmol/L or random plasma glucose [RPG] ≥11.1 mmol/L and<18 mmol), the immediate intervention is counselling on diet and physical activity (see Fig. 4). It is also important to obtain a full medical history, including for cardiovascular disease, given the higher risk of both micro- and macrovascular complications among people with diabetes and the need for prevention and management. Blood glucose levels should be re-assessed by a health worker after 1 month or immediately symptoms appear. Further details are provided in Fig. 4.
Management of type 2 diabetes in people with TB should be provided according to existing guidelines (33). While glycaemic control to achieve an HbA1c of about 7% is generally recommended, a more lenient HbA1c target (e.g. < 8%) might be assigned to people with diabetes who have markedly elevated glucose levels and TB, which would be more tolerable in the short term to achieve the aim of good, consistent glycaemic control. A healthy diet to achieve or maintain a normal body weight and regular physical activity are the mainstays of diabetes management. Tailored advice should be provided on a balanced diet, physical activity, weight management, smoking cessation and harmful use of alcohol as appropriate.
Glucose-lowering medication might also be necessary. Metformin is the recommended initial glucose-lowering medication for people who do not achieve the desired glycaemic control with diet and physical activity. A second-generation sulfonylurea (preferably gliclazide) may be used as initial first-line treatment when metformin is contraindicated (i.e. estimated glomerular filtration rate < 30 mL/min per 1.73 m2 ) or not tolerated. If diet, physical activity and metformin do not control glycaemia, a second-generation sulfonylurea may be combined with metformin. If this does not control hyperglycaemia, treatment with human insulin may be considered. If other glucose-lowering medication is more affordable than human insulin, options such as dipeptidyl peptidase 4-inhibitors, sodium glucose co-transporter 2 inhibitors or pioglitazone could be used before insulin in cases of treatment failure with metformin and gliclazide.
Fig. 4. Protocol for control of blood glucose in people with type 2 diabetes
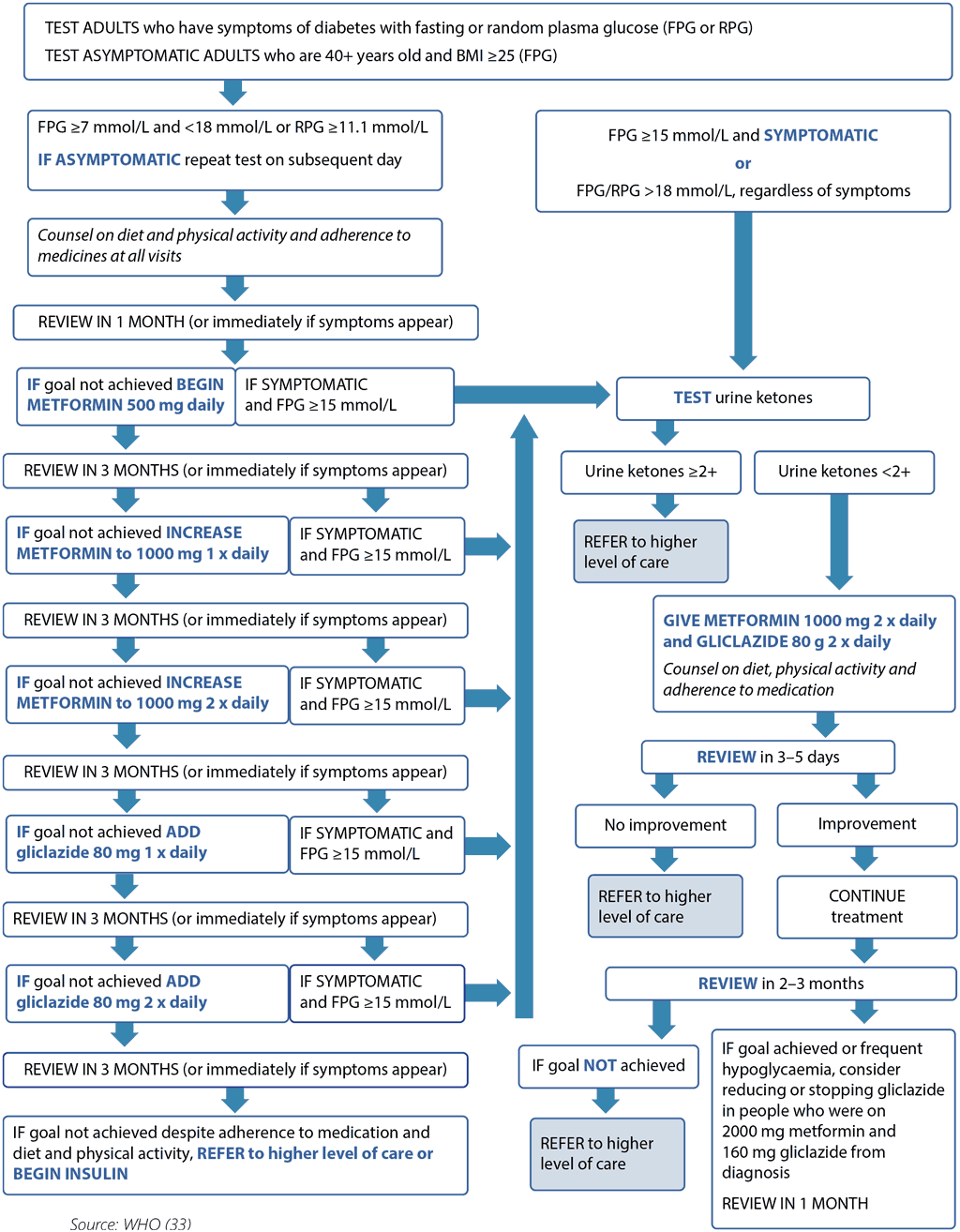
Further guidance on the management of type 2 diabetes, including the prevention and management of complications, is provided in the WHO guidance, Diagnosis and management of type 2 diabetes (HEARTS-D) (33). Potential interactions between TB medication and glucose-lowering medication should always be considered (see section 3.3), potentially with additional monitoring. As the glucose-lowering effect of insulin is not affected by anti-TB medications, some experts recommend initiation of insulin earlier during TB treatment than the WHO protocol (Fig. 4) recommends in order to achieve faster glycaemic control and bacteriological sputum conversion and to prevent drug–drug interactions. Although not recommended by WHO as standard practice, this may be considered within the context of individual needs and clinical judgement (120).
4.2.2 Management of type 1 diabetes
Globally, type 1 diabetes represents about 2% of the estimated diabetes burden, ranging from < 1% in certain Pacific countries to > 15% in northern European populations (179). The type of diabetes cannot, however, always be determined at diagnosis, and initial treatment decisions should be based on clinical presentation and plasma glucose values. Newly diagnosed individuals with clinically suspected type 1 diabetes should be referred to a higher level of care, as type 1 diabetes is usually not managed in primary care facilities (33). WHO guidelines recommend use of human insulin (short- and intermediate-acting) to manage blood glucose in adults with type 1 diabetes. Long-acting insulin analogues might be considered as a last resort to control blood glucose levels in adults with type 1 diabetes who have frequent severe hypoglycaemia when taking human insulin. There is limited evidence that insulin analogues are more effective, and human insulin is associated with better resource use (180). People with type 1 diabetes who are on insulin should be offered self-monitoring of blood glucose. Self-monitoring and self-adjustment of dosage are recommended in type 1 diabetes according to an agreed plan with a health professional (34,181,182).
4.2.3 Management of complications of diabetes
In addition to achieving glycaemic control, it is also important to consider holistic monitoring and care for complications of diabetes. The two most common acute complications are hypoglycaemia (abnormally low blood glucose) and hyperglycaemic emergencies, including diabetic ketoacidosis and hyperosmolar hyperglycaemic state. Additionally, diabetes can cause microvascular and macrovascular complications. Microvascular complications such as diabetic retinopathy, nephropathy and neuropathy are typically silent until advanced and can often be identified at screening. Macrovascular complications such as coronary artery disease and cerebrovascular disease can be prevented with comprehensive control of cardiovascular disease risk factors by use of antihypertensives, statins and antiplatelet medications. Algorithms for the prevention and management of these conditions among people with diabetes are summarized elsewhere (34). If diabetes is managed in a TB clinic, the health-care workers should receive continuous training and mentoring about the risks of clinical deterioration of patients with diabetes and about the criteria for referral to specialist services and for seeking emergency care.
4.2.4 Side-effects and drug–drug interactions of glucose-lowering medication
Special considerations for use of diabetes medication during TB care are discussed in section 3.3.1. Side-effects can reduce adherence to prescribed medication, and drug–drug interactions can reduce its efficacy. TB clinic workers should be aware of the risks and should be trained to respond accordingly. Through task shifting and with appropriate training, community health workers or peer supporters may be able to assist. For example, they could enquire about adherence to anti-TB and glucose-lowering medications, help to resolve any difficulties experienced and provide information about prescriptions.
4.2.5 Considerations for integrated care and linkage to care after completion of TB treatment
To prevent nosocomial transmission of TB to other people attending a diabetes clinic, care for the two diseases should ideally be provided in the TB clinic, when feasible. Provision of care in one location is also more convenient for the person receiving care. Lessons learnt from the health system response to COVID-19 may be used to inform the use of virtual technology, including provider-to-provider telemedicine to support co-management of diabetes within TB care (183). Co-management of TB and diabetes in the same clinic may improve treatment outcomes and ensure timely identification and management of drug–drug interactions and side-effects (13,53,56). For more information on models of TB and diabetes care, see section 2.
If diabetes is managed in a TB clinic, the individual with TB should be referred appropriately for continued care for diabetes at the end of TB treatment, with transfer and linkage of the relevant medical records. Counselling should be provided to ensure that the person understands that, while they may be cured of TB, diabetes is a lifelong condition, which will require ongoing management. Monitoring of individuals transferred to diabetes care should be a part of collaborative routine monitoring and evaluation in TB and diabetes clinics to ensure continuity of care.

 Retour
Retour